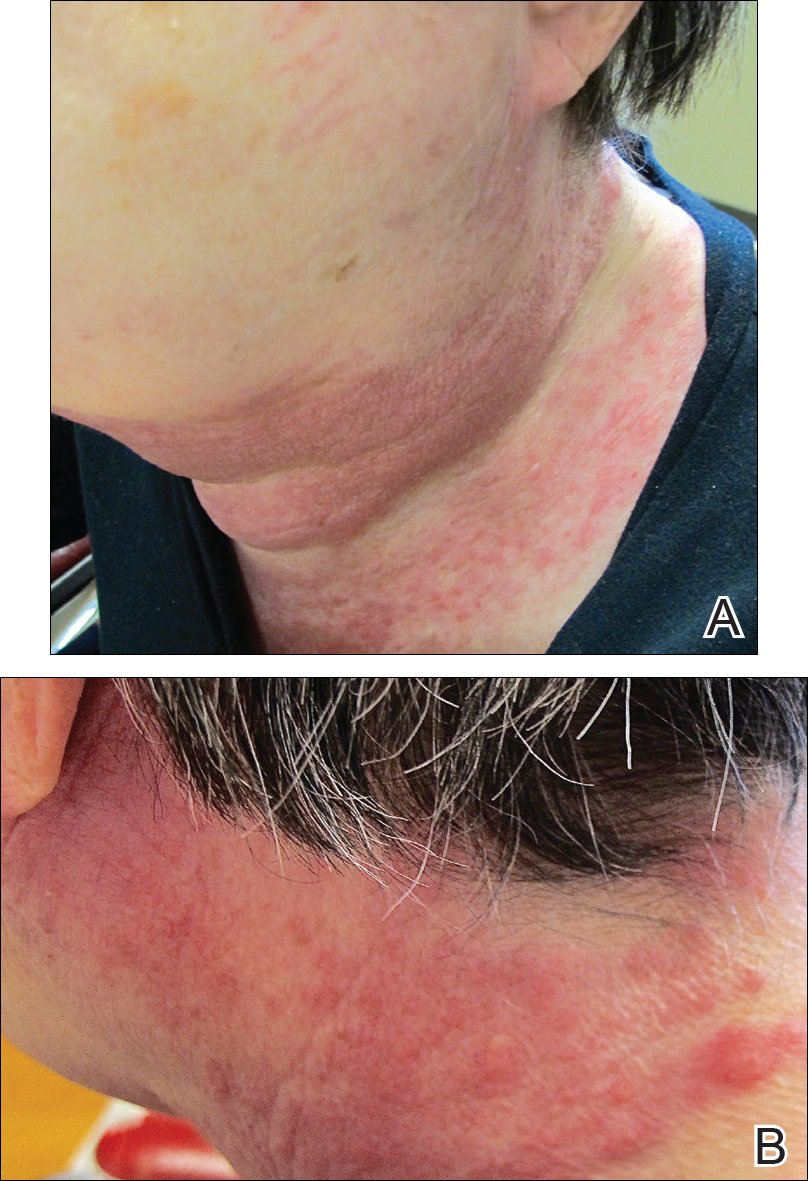
3 The presentation of adult-onset eczema is more heterogenous, with wider variation in lesion morphology and distribution, including higher rates of nummular and prurigo lesions and less involvement of classic flexural surfaces. 2 In childhood it begins as weeping vesicles, progressing to dry, scaling papules and plaques, finally becoming lichenified, hypertrophied plaques from scratching. 1 It is an inflammatory, spongiform dermatitis with a pruritic, erythematous, scaly rash affecting flexural surfaces that often begins in childhood, holding a relapsing–remitting course. Six months later, he had moderate improvement of his rash ( figure 2).Ītopic dermatitis, or eczema, affects 3%–7% of adults in the USA. However, due to concern for poor daily compliance was instead given mycophenolate mofetil. He started topical triamcinolone 0.1% ointment and emollients with wet wraps. Punch biopsy showed spongiotic dermatitis, consistent with atopic dermatitis. A primary immunodeficiency may also account for the rash, weight loss and lymphadenopathy, although immunoglobulin levels and flow cytometry were normal. The arterial thrombosis responsible for the patient’s cyanotic and gangrenous foot, as well as the severe rash, weight loss and diffuse lymphadenopathy raised concern for malignancy, particularly a cutaneous T-cell lymphoma (CTCL). Liver ultrasound revealed heterogeneous parenchyma with a nodular contour and ascites, suggesting chronic liver disease. Duodenal biopsies revealed scalloping and atrophic mucosa, but MR enterography revealed no small bowel inflammation. He subsequently underwent below-the-knee amputation with rapid improvement on antibiotics, and was started on anticoagulation and aspirin for the numerous atherothrombi.Ī malabsorptive process was suspected due to severe hypoalbuminaemia, weight loss and deficiencies of folate, selenium, zinc and multiple vitamins which could have contributed to the rash. CT-angiogram with 3-vessel run-off in the left lower extremity revealed mediastinal, para-aortic and bilateral axillary and inguinal lymphadenopathy, and non-visualisation of the anterior, posterior tibial and common peroneal arteries and numerous non-occlusive calcified and non-calcified thrombi within the lumens of the infrarenal abdominal aorta, common iliac artery and left common femoral artery. Notable labs included albumin of 1.3 g/L, leucocytosis to 17×10 9/L and lactate of 3.2 mmol/L. His left foot was cyanotic, tender and pulseless with gangrene of the third digit. He was ill appearing with diffuse xerosis and lichenified, erythematous, scaly plaques of the extremities, back, chest and abdomen with overlying excoriations, erosions and secondary crusting ( figure 1). On examination, he was afebrile, tachycardic to 140 beats/min, and hypotensive to 98/65 mm Hg. He was a pack-a-day smoker and denied alcohol use. He denied any history of allergies, food sensitivities, asthma, hay fever, atopic dermatitis or childhood rashes. Over the last year, he had the onset of a whole-body pruritic rash and unintentional 25 kg weight loss. A 45-year-old previously healthy man presented to the hospital with acute left foot pain with numbness, coldness, blue discoloration, a blackened third toe and chills for 4 days.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
